Diabetes
What is Diabetes?
Diabetes (also referred to as diabetes mellitus) is a long-term condition where the amount of glucose (sugar) in the blood is too high. This happens when the pancreas does not produce any insulin, enough insulin or the body is resistant to it. Insulin acts like a key to unlock the pathway to allow glucose to move from the blood into the cells to provide energy. Diabetes affects approximately 4.3million people in the UK. Approximately 8% of people with diabetes will have Type 1 and around 90% will have Type 2. The other 2% accounts for other types of diabetes. please click here.
For more information on diabetes please follow the link to www.diabetes.org.uk/about-diabetes.
An easy read leaflet on diabetes can be found by clicking here.
Type 1 Diabetes
Type 1 diabetes cannot be prevented. It is caused by a fault in the body’s immune response system, where the cells responsible for producing insulin are targeted and destroyed by mistake. People with type 1 diabetes will always require insulin therapy.
Type 1 diabetes | Diabetes UK
Type 2 Diabetes
Type 2 diabetes occurs when the pancreas is not producing enough insulin and/or the body resists to the action of insulin (insulin resistance). People with type 2 diabetes are usually managed with lifestyle advice and/or oral medications. Sometimes injectable therapies (including insulin) are required to help manage type 2 diabetes as it progresses. It is possible in some circumstances that you can get your diabetes into remission. This is achieved when your long-term blood sugar (HbA1c) is less than 48mmols for at least 3 months after stopping all diabetes medication.
Type 2 diabetes | Diabetes UK
Early Onset Type 2 Diabetes
People aged 18-39yrs who develop Type 2 diabetes need special consideration. This is because they will be living with the condition for longer and are therefore more at risk of developing complications sooner.
Further resources can be found by clicking below:

Diabetes in Pregnancy
Women with early onset Type 2 diabetes will also need specialised care in pregnancy. It is important NOT to get pregnant when your sugar levels are high as this can be dangerous and damaging to both the unborn child and mother. If you are planning a pregnancy the following things are very important:
- Ask your GP for referral to Pre-Conception clinic at the hospital for specialist assessment and advice
- Make sure you are up-to date with your diabetes checks (9 care processes)
- Diabetes increases the risks in pregnancy, but by planning and seeking advice you can reduce the risks and have a healthy and enjoyable pregnancy.
- A pregnancy should be planned carefully, and you should remain on contraception until your HbA1c is in the target range.
- In general women with diabetes can choose from the full range of contraception. Discuss with your practice nurse or GP about the best contraception for you.
- Managing your glucose levels well and reducing your HbA1c to target before getting pregnant will increase your chances of having a healthy pregnancy.
- You will need a prescription for folic acid 5mg. Women with diabetes need a higher dose of folic acid.
- You will benefit from taking 10mcg of Vitamin D which you can buy over the counter.
- Ask the GP to review your medications as some routine medications taken by women with diabetes may harm your baby.
- Eat a healthy balanced diet and take regular exercise. You are advised to stop smoking and drinking alcohol before you get pregnant. Your GP can support you with this.
- Don’t panic if you have an unplanned pregnancy. Phone the diabetes centre at Sheffield Teaching Hospitals 01142714445 and contact your GP surgery.
Contraception - There are several choices of contraception. Follow this link for more information Contraception - NHS. If you have complications related to your diabetes such as damage to your eyes, kidneys or nerves, your contraception options may be more limited. Discuss the best contraception choice for you with your healthcare team.
Type 1 diabetes and contraception | Diabetes UK
Microsoft Word - Diabetes UK Information Prescription - Contraception and pregnancy.docx
Children with Diabetes
Children with diabetes will be under the care of the Sheffield Children’s Hospital.
The Diabetes team specialise in working with children up to 18 years of age with all types of diabetes:
- Type 1 diabetes
- Type 2 diabetes
- Cystic fibrosis related diabetes
- Steroid -induced diabetes
- Uncommon diabetes types such as maturity onset diabetes of the young (MODY)
Children’s diabetes services enquiries call 0114 271 7320 (8am – 4pm)
When families need to call the hospital for ‘out of hours’ diabetes advice, you should call the SCH switchboard on 0114 271 7000 and ask to be put through to the senior medical doctor on call.
Diabetes service - Sheffield Children’s NHS Foundation Trust
Young Persons Diabetes Service (16-20yrs)
A person who is newly diagnosed with diabetes who is more than 16 years old would usually be referred to adult services at the Northern General Hospital.
Digibete is an app for the who family and community managing type-1 diabetes. It is clinically approved by NHS experts. Please follow the link here for further information.

The young person’s diabetes clinic at the Northern General Hospital is held on the 1st and 3rd Wednesday afternoon of each month. For more information, please click on the link below.
Transition to the young person’s Diabetes service in Sheffield - Resource Library - Sheffield Children's NHS Foundation Trust
Steroid-Induced Diabetes/Hyperglycaemia (high blood sugar because of taking steroid medication)
Steroids are artificial versions of hormones that are naturally produced by your body. They reduce inflammation in your body and can help to treat conditions such as severe asthma/COPD, cystic fibrosis, arthritis, inflammatory bowel disease, other inflammatory conditions and are also used in some cancer treatments. These are not the same as anabolic steroids which increase body muscle mass.
Steroid-induced diabetes
Steroids can cause high blood glucose (sugar) levels. Some people who take steroids can develop (steroid-induced) diabetes. Sometimes dietary changes are enough to control the blood sugar. Other times additional medication is required. Steroid-induced diabetes may or may not resolve when the steroid medication stops.
Steroid-induced hyperglycaemia
Steroids can also cause a further increase in blood sugar levels for those who already have diabetes, and medication may need to be adjusted to maintain good control. If you are taking medium to high-dose, repeated courses or prolonged courses of steroids you should have access to blood sugar testing with a glucose monitor.
Please follow the link below for more information: Steroid-induced diabetes | Diabetes UK
Gestational Diabetes
If you have a history of Gestational Diabetes (diabetes in pregnancy) you are at increased risk of developing type 2 diabetes in the future. It is therefore important you have an annual blood test (HbA1c). You can book this blood test at the surgery, attend the drive through service at Longley or attend the Phlebotomy department at the Hallamshire or Northern General Hospitals.
You can find out more about gestational diabetes here: What is gestational diabetes? | Causes & symptoms | Diabetes UK
You can take control of your risk of diabetes by moving more, improving your diet and maintaining a healthy weight longer term and the Diabetes Prevention Programme (DPP) can help with this. You can self-refer for this free NHS service and be seen online or in person. Please take a look at the website for more information https://healthieryou.reedwellbeing.com/gestational-diabetes/ (scan the QR code below) or chat to your nurse or GP at your next appointment.
It is important to remember that if you develop any signs or symptoms of diabetes, such as increased thirst, thrush infection, fatigue or passing lots of urine that you let your GP know promptly so they organise a test and support you.

Scan the QR code for more information on how NHS Healthier You can provide support after gestational diabetes or pre-diabetes through the Diabetes Prevention Programme.
.
Am I at risk of Diabetes?
If you would like to see if you are at risk of developing diabetes, you can use the button below to fill in a short questionnaire. If you have any concerns regarding this then you should contact your GP Practice for further advice.

Pre-Diabetes
This diagnosed when you have a HbA1c between 42- 47mmols. If your level is in this range it means that you are at higher risk of developing Type 2 diabetes. Please see the section on the Diabetes Prevention Programme (DPP).
.
How do I look after my Diabetes?
If you are excessively thirsty, passing a lot or urine or you feel unwell, please seek immediate medical attention. You can call your GP surgery or NHS 111 for further advice and guidance. If you have been diagnosed with Type 1 diabetes or are under the care of the diabetes specialist nurses, you can also call the diabetes centre on 0114 271 4445.
Your diabetes will be reviewed at the surgery at least once a year. Patients will need to book a 20-minute appointment for monitoring tests. This will include blood sampling, foot check, blood pressure and height and weight measurements. You will then need a follow-up appointment with the Practice Nurse to review the results, discuss your medication and to agree your ongoing management plan for your diabetes. Blood tests and other monitoring may be required more often to improve control or check levels after medication changes.
.
What to expect from your diabetes review
During your annual diabetes review, the clinician will focus on the 9 key areas below, as well as other life style issues, to help you improve your diabetes control.
1. HbA1c
This is a blood test that shows your average blood sugar over a period of 3 months. Diabetes is diagnosed when you have two readings above 48mmols. The nurse will discuss your individual HbA1c target with you during your review.
2. Cholesterol
Your cholesterol level is checked by a blood test at least once a year. Depending on your result, your age and your type of diabetes, you may be offered a tablet called a statin. A statin helps to lower your cholesterol level and reduce your risk of having a cardiovascular event like a heart attack or a stroke. You can find more information on statin medication here.
3. Blood Pressure
If you have diabetes, it is very important to keep your blood pressure in a healthy range to reduce your risk of complications. When your heart pumps it creates pressure in your blood vessels. The top number is the pumping pressure (systolic). The bottom number is the resting pressure (diastolic). Your blood pressure can vary throughout the day. At least half of heart attacks and strokes are associated with high blood pressure. It is also a major risk factor for chronic kidney disease, heart failure and dementia.
4. Kidney Function
Raised blood sugar levels can be damaging to the tiny blood network and filters in your kidneys. This is called nephropathy. Your kidney function should be monitored by a blood test at least once a year. This may need testing more often if your kidney function is altered or you are taking certain medications.
5. Urine ACR
High blood pressure and diabetes can also affect your kidney filters and sometimes causes protein to leak out into the urine. This is monitored at least once a year by a urine test called an ACR (Albumin Creatinine Ratio). Urine ACR Leaflet
These blood and urine tests allow problems to be recognised early and treated to reduce the risk of long-term complications.
6. Eye Screening (Retinopathy Screening)
Diabetic eye screening is offered in a variety of locations throughout the city, including certain GP surgeries and hospitals. Sometimes additional clinics are offered more locally at the SWFC stadium.
All people aged 12 and over with diabetes (type 1 and 2) are offered eye screening. You will be invited again either after 12 months or 2 years depending on your eye screening result. If any treatment of further investigations are required, you will be offered a referral to opthalmology.
The only exceptions to routine eye screening are people with diabetic eye disease who are already under the care of an ophthalmology specialist.
The screening test usually takes around 30 minutes. On arrival some drops will put into your eyes to dilate your pupils so that photographs of the back of your eyes can be taken with a specialised camera. As it takes a little while for your eyes to return to normal after the test so you will not be able to drive for a few hours.
Diabetic eye screening does not replace regular eye examinations and it is important to attend both. If you are anxious about attending your eye screening appointment or worried about any results, please speak to your GP or Practice Nurse.
To book your eye screening appointment, please call 0114 226 5475.
Diabetic eye screening - Sheffield Teaching Hospital
Diabetic eye screening - NHS - Includes explanation video of your eye screening appointment
Diabetic eye screening | Retinopathy | Diabetes UK
Diabetic eye screening: information leaflets - GOV.UK - Includes easy-read leaflets
Sheffield Teaching Hospitals - Diabetes - Includes video
7. Foot check
These tests are to make sure you have good circulation to your feet and to check for any signs of nerve damage (neuropathy). For further information about neuropathy you can click here. You will be offered a foot check at least once a year. The nurse will feel for your foot pulses and will sometimes use a special machine called a doppler to hear the foot pulses. The sensation in your feet will also be checked with a small instrument called a monofilament. You can see how a foot check is done by watching the video here.
It is also important that you check your own feet on a daily basis for any changes, breaks in the skin or signs of infection. You should contact the surgery promptly with any changes (call 111 if the surgery is closed). Here are some tips to keep your feet healthy:
- Moisturise your feet daily to minimise the risk of hard and/or cracked skin as this can increase the risk of infection and development of foot ulcers.
- Do not to moisturise between the toes or the toenails as this may encourage fungal infections.
- It is not advisable to remove/cut off hard skin yourself or use corn plasters.
- File your nails once a week instead of cutting your nails.
- Any hard skin can be filed gently with an emery board.
- Good supportive footwear is very important to reduce the risk of foot problems.
It is estimated that between 5-7% of people with diabetes will have a diabetic foot ulcer at some point in their lives. This risk can be reduced by keeping good control of your blood sugar and blood pressure, not smoking, checking your feet daily and seeking prompt medical attention with any changes.
Diabetes UK Foot Check Leaflet
If your feet are assessed to be higher risk, you will be offered a referral to the podiatry service, who are more specialised in foot care.
If you have an acute foot problem, such as an infection or an ulcer, then you may be referred directly to the foot clinic at the hospital.
8. Body Mass Index (BMI)
Keeping a healthy weight when you have diabetes helps to protect and reduce long-term risk for your heart, eyes kidneys and feet. A normal BMI in adults is 18.5 to 24.9 kg/m2. This range is a guide to indicate a healthy weight for your height. A BMI below 18.5 is considered to be underweight and a BMI above is considered to be overweight. You can calculate your own BMI by clicking the link here.
9. Smoking
Smoking increases you risk of heart attacks, strokes, cancer and other serious health conditions. This risk increases further if you smoke and have diabetes. Please follow the links below for advice and support to stop smoking.
https://sheffield.yorkshiresmokefree.nhs.uk/
https://www.diabetes.org.uk/living-with-diabetes/life-with-diabetes/help-with-giving-up-smoking
What could happen when you quit smoking - Better Health - NHS
10. Lifestyle
Alcohol - The government guideline recommends you limit your alcohol intake to a maximum of 14 units spaced over a minimum for 3 days. It is also recommended to have a few days each week without any alcohol. It is more important to be aware of your alcohol intake if you have type 2 diabetes as it is high in calories. It is advisable to reduce your alcohol intake if you are trying to lose weight.
https://likewisesheffield.org.uk/
https://alcoholchange.org.uk/
Physical Activity - Regular physical activity has many health benefits to improve your quality of life. It helps to maintain a healthy weight, manages stress and is associated with better sleep. It is also important in managing your diabetes and reducing the risk of heart attacks and strokes. In addition it reduces the risk of falls, depression, dementia, joint & back pain and some cancers.
Benefits of exercise - NHS
Healthy Living for people with type 2 diabetes - NHS
https://www.stepoutsheffield.co.uk/
Diet - Eating a regular healthy diet that is low in fat, sugar and salt is important for general health benefits and maintaining a healthy weight. It also helps to control your diabetes and to reduce your risk of long-term complications. Please follow the link below for advice on carbohydrates and other food types, healthy swaps, understanding food labels, recipes, meal planning, shopping on a budget and during Ramadan.
Healthy eating | Living with diabetes | Diabetes UK
The Eatwell Guide - NHS
Diabetes and Ramadan | Fasting | Diabetes UK
Wellbeing – Diabetes is a long-term condition that people sometimes find challenging to accept and manage alongside the stress of everyday life. If you feel this is affecting your well-being please speak to your GP or nurse. You can also self-refer to Sheffield Talking Therapies who offer a wide range of services including help with long-term conditions.
Health and Wellbeing Service | NHS Sheffield Talking Therapies
Mindfulness for Health
.
Courses and Referrals
MoreLife
You can refer yourself to this 12-week programme if you are an adult with a BMI above 25 or above 23.5 if you have a Black/Asian or other ethnicity. You can choose to do the programme face-to-face or online and it covers mindful eating, stress and emotional eating Home Page - Morelife UK
Move Well - Move More
Many people with health conditions find that being active helps them manage their condition and symptoms, as well as improving their general well-being. You can self-refer to this by clicking on the link below:
Move Well — Move More Sheffield
SWFC Community Team
The SWFC community programme is the charitable arm of the football club, working with 4 key areas health and wellbeing, education, participation and youth and integration. Latest stats from our impact report are as followed
The health team offer a wide variety of programmes health specific, and community based such as
- Osteoarthritis classes
- Post Natal Fitness
- Walking football
- Steps classes
- Gym memberships
- Weight Management programmes
- Walking group
For more information, please follow this link:
Sheffield Wednesday FC Community Programme | Health & Gym | Shop | Abler
Or contact health@swfc.co.uk
Step-Out Sheffield
This is a city-wide programme FREE WEEKLY WELLBEING WALKS. This is a volunteer led scheme, delivering weekly walks at 22 different sites across the city, including within our locality.
Telephone: 07505639524 E-mail: https://www.stepoutsheffield.co.uk/
DESMOND course
For people with Type 2 Diabetes (Diabetes Education and Self-Management for On-going and Newly diagnosed Diabetes) to increase your knowledge skills and confidence to manage your own diabetes.
https://publicdocuments.sth.nhs.uk/PIL4130.PDF
DAFNE Course
DAFNE stands for Dose Adjustment For Normal Eating. It aims to help adults with type 1 diabetes lead as normal a life as possible, whilst also maintaining blood glucose levels within healthy targets, to reduce the risk of long-term diabetes complications.
Home - DAFNE
Diabetes Prevention Programme
This programme lasts for 9 months and consists of fortnightly sessions for 4 sessions then monthly. It is offered to those with pre-diabetes or a history of diabetes in pregnancy (gestational diabetes). There are face-to-face or digital sessions. On-line tailored sessions are also available if your vision or hearing is impaired or if you have a history of gestational diabetes. Please contact the practice if you would like to be referred. Please follow the link for further information:
https://healthieryou.reedwellbeing.com/about-the-programme/
Type 2 Diabetes Remission Programme
Research has shown that a 3-month specially formulated diet comprising of total diet replacement products including soups and shakes, followed by healthy lifestyle support helps people living with type 2 diabetes to lose weight, improve their blood sugar levels, reduce diabetes-related medication and, in almost half of participants, put their type 2 diabetes into remission. There are specific criteria that needs to be met before being accepted onto the programme. The products and the programme are FREE. You can check your eligibility from information in the link below. Please contact your practice if you would like to be referred.
South Yorkshire: NHS Type 2 Diabetes Path to Remission - Momenta Newcastle
NHS Digital Weight Management Programme
This programme is available to adults with diabetes (Type 1 or Type 2) and/or hypertension (high blood pressure) with a raised BMI (body mass index). It is a an on-line behavioural and lifestyle programme over 12 weeks with three different levels of support which is allocated after assessment. Please contact the surgery if you would like to be considered for referral.
Information Video: Bing Videos
NHS Weight Loss APP
This is a self-upload APP for adults. It can be used with a smart phone or computer and gives digital support with calorie counting, weight monitoring and tracking activity with a flexible 12-week plan:
https://www.nhs.uk/better-health/lose-weight/
Carbsmart Course
.
Hypos and Driving Rules
Hypos (Hypoglycaemia)
This happens when your blood sugar level is too low (less than 4mmols) and must be treated immediately. If a hypo is indicated on your continuous glucose monitor (e.g. Libre, Dexcom) it is always important to check with a finger prick test.
Causes of a hypo include:
- Too much insulin or certain medications
- Missed or delayed meals
- Less carbohydrates than normal
- Increased exercise
- Heat
- Too much alcohol
- Lumpy injection sites
- Not mixing insulin
Common symptoms of a hypo are:
- sweating/pale
- feeling shaky /dizzy/wobbly or anxious
- palpitations
- tingling lips
- feeling hungry
- loss of energy/weakness
If these symptoms are not treated immediately and blood sugar levels continue to fall symptoms can worsen:
- blurred vision
- loss of concentration/confusion
- slurred speech
- change in behaviour
Please see the hypo card below on what to use to treat a hypo. This treatment may need to be repeated if your blood sugar is still less than 4mmols after 15 minutes.
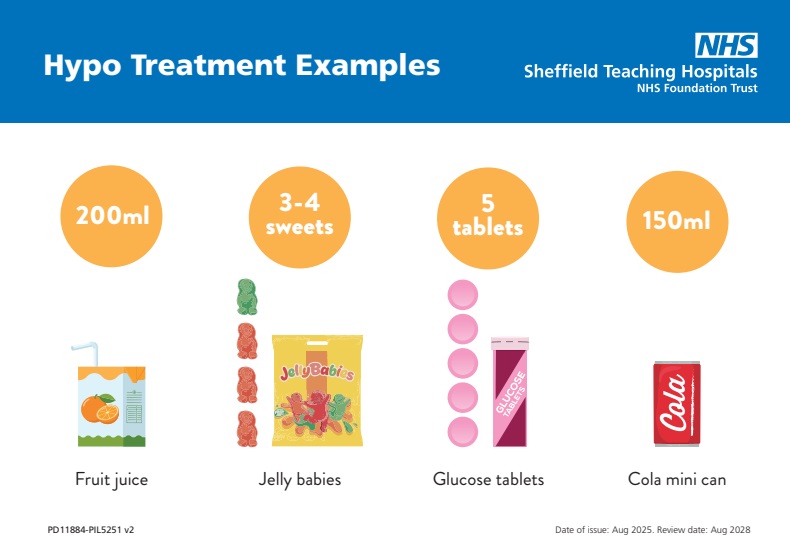
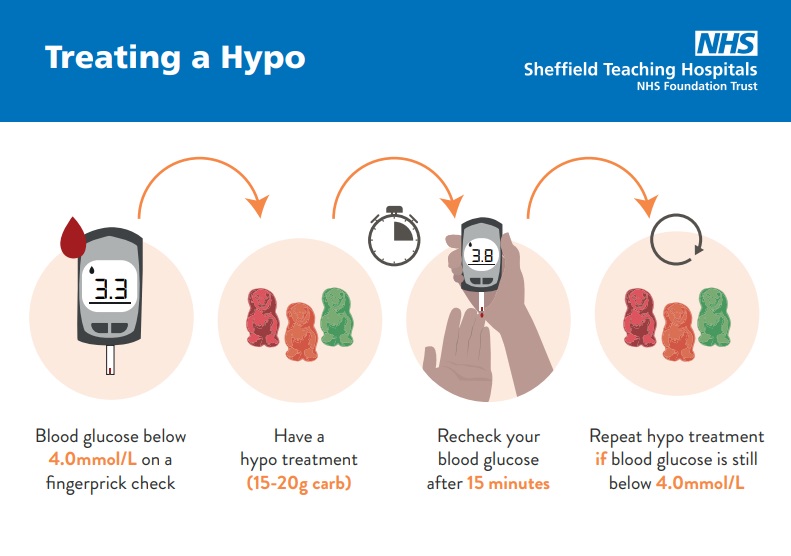
After treating your hypo, it is recommended to either bring your next meal forwards or have a carbohydrate snack
For example:
- A piece of fruit
- Cereal bar
- Slice of bread or toast
- 2 biscuits
- Small bowl of cereal with milk
Ways to keep yourself safe:
- Eat regular healthy meals
- Carry a hypo treatment with you
- Keep alcohol to a sensible amount.
- Check you blood sugar more often if you are drinking alcohol or exercising
- Carry diabetes ID with you
- Make sure family and friends know that you have diabetes & know how to help if you have a hypo
- Check your blood sugar more often after having a hypo as you are at higher risk of having another one.
Information Leaflet: A5_Hypo_TREND.pdf
Driving
- Remember ‘5 to drive’– your blood sugar must be above 5 mmols to legally drive
- Carry testing equipment and a hypo treatment in your car
- If you are on a longer journey test your blood sugar every 2 hours
- If you have hypo symptoms when driving – stop the car – remove the keys from the ignition – move to the passenger seat - test your blood sugar – if less than 4mmols treat with a hypo treatment – do not drive again for at least 45 minutes after your blood sugar has come back above 4mmols– check again that your level has risen above 5 mmols before driving again.
- There are special considerations if you drive an HGV/bus. Please see the DVLA link below for further information.
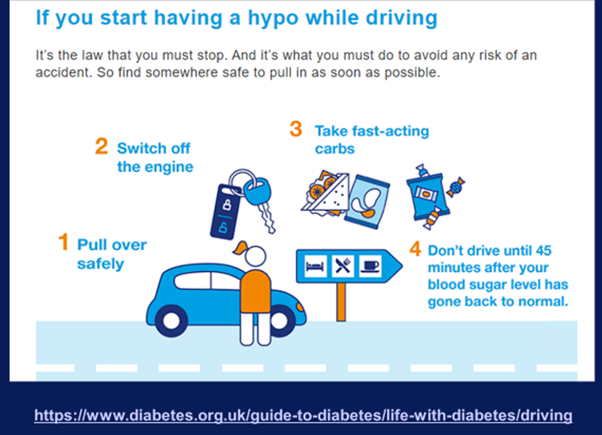
For further information please visit:
Diabetes and driving - GOV.UK
www.gov.uk/dvla
http://www.diabetes.org.uk/t2-driving
https://www.diabetes.org.uk/guide-to-diabetes/life-with-diabetes/driving
Sick Day Rules
If you are feeling unwell this may affect your diabetes and how much medication you need to take. Please follow the links below for further information.
If you are excessively thirsty, passing a lot or urine or you feel unwell, please seek immediate medical attention. You can call your GP surgery or NHS 111 for further advice and guidance. If you have been diagnosed with Type 1 diabetes or are under the care of the diabetes specialist nurses, you can also call the diabetes centre on 0114 271 4445.
Sick day rules
https://www.drwf.org.uk/sites/default/files/managing_diabetes_when_you_are_ill_v7.0_a4.pdf
Type 1 Diabetes - Illness
https://trenddiabetes.online/wp-content/uploads/2020/03/A5_T1Illness_TREND_FINAL.pdf
Type 2 Diabetes - Illness
https://trenddiabetes.online/wp-content/uploads/2020/03/A5_T2Illness_TREND_FINAL.pdf
.
Useful Telephone Numbers
Diabetes Centre: 0114 271 4445
Diabetic Eye Screening: 0114 266 5475
Community Podiatry: 0114 307 8200
Stop Smoking Services (Smokefree Sheffield): 0114 553 6296 or 07833 048200
Likewise Alcohol Services: 0114 308 7000
.
Useful Links
Diabetes UK
https://www.diabetes.org.uk/
Dementia
https://trenddiabetes.online/wp-content/uploads/2021/02/A5_Dementia_TREND.pdf
DKA
https://trenddiabetes.online/wp-content/uploads/2019/04/A5_DKA_2019_TREND.pdf
Eye Screening
https://www.gov.uk/government/collections/diabetic-eye-screening-information-leaflets
Genital Healthy Living
https://trenddiabetes.online/wp-content/uploads/2019/07/A5_Genital_TREND.pdf
https://healthyliving.nhs.uk/
Heart UK
https://www.heartuk.org.uk/cholesterol/overview
Hypo
https://trenddiabetes.online/wp-content/uploads/2020/10/A5_Hypo_TREND.pdf
Insulin
https://trenddiabetes.online/wp-content/uploads/2020/06/A5_insulin_TREND_v13.pdf
Menopause
https://trenddiabetes.online/wp-content/uploads/2021/08/A5_Menopause_TREND.pdf
NHS England
https://www.youtube.com/playlist?list=PL6IQwMACXkj3EDhR24rNE8EsZJDw_Cbfm
Older Person
https://trenddiabetes.online/wp-content/uploads/2020/10/A5_Older_Person_TREND.pdf
PEI
https://trenddiabetes.online/wp-content/uploads/2020/05/A5_PEI_TREND_v4.pdf
Patient.info DM 1
https://patient.info/diabetes/type-1-diabetes
Patient.info DM 2
http://patient.info/health/type-2-diabetes
Patient.info DM + Unwell
https://patient.info/diabetes/diabetes-mellitus-leaflet/diabetes-and-illness
Driving
https://www.diabetes.org.uk/guide-to-diabetes/life-with-diabetes/driving
Foot
https://trenddiabetes.online/wp-content/uploads/2021/08/A5_Foot_TREND.pdf
Footcare
https://patient.info/diabetes/diabetes-mellitus-leaflet/diabetes-foot-care
T1Illness
https://trenddiabetes.online/wp-content/uploads/2020/03/A5_T1Illness_TREND_FINAL.pdf
T2Illness
https://trenddiabetes.online/wp-content/uploads/2020/03/A5_T2Illness_TREND_FINAL.pdf
Hypoglycaemia
http://patient.info/health/dealing-with-hypoglycaemia-low-blood-sugar
Hyperglycaemia
https://patient.info/diabetes/type-1-diabetes/dealing-with-hyperglycaemia-high-blood-sugar
Hypertension
https://patient.info/diabetes/diabetes-mellitus-leaflet/diabetes-and-high-blood-pressure
On Insulins
https://patient.info/diabetes/type-1-diabetes/insulins
Lifestyle
http://patient.info/health/diabetes-healthy-eating-sheet
https://movingmedicine.ac.uk/wp-content/uploads/2025/09/PACE-up-MM-edit-2025.pdf
https://movingmedicine.ac.uk/wp-content/uploads/2025/06/Patient-workbook.pdf
Nephropathy
http://patient.info/health/diabetic-kidney-disease-leaflet
Neuropathy
http://patient.info/health/peripheral-neuropathy-leaflet
NHS Choices
http://www.nhs.uk/conditions/diabetes/pages/diabetes.aspx
Pregnancy
http://patient.info/health/pregnancy-and-diabetes
Retinopathy
http://patient.info/health/diabetic-retinopathy-leaflet
Share the Pressure
https://sharethepressure.com/
Sick day rules
https://www.drwf.org.uk/sites/default/files/managing_diabetes_when_you_are_ill_v7.0_a4.pdf
Steroids
https://trenddiabetes.online/wp-content/uploads/2020/10/A5_Steroids_GRX_TREND.pdf
Substance
https://trenddiabetes.online/wp-content/uploads/2020/06/A5_Substance_TREND.pdf
Travel - Diabetes UK
https://www.diabetes.org.uk/travel
Travel - NHS.uk
http://www.nhs.uk/Livewell/travelhealth/travelling-with-diabetes.aspx
Video Resources
http://www.thesounddoctor.org/
Wellbeing
https://trenddiabetes.online/wp-content/uploads/2020/10/A5_Wellbeing_TREND.pdf
What is Diabetes
https://www.youtube.com/watch?v=4SZGM_E5cLI
Living Well
www.diabetes.org.uk/guide-to-diabetes/managing-your-diabetes/information-prescriptions/
Learning Zone
https://learningzone.diabetes.org.uk/